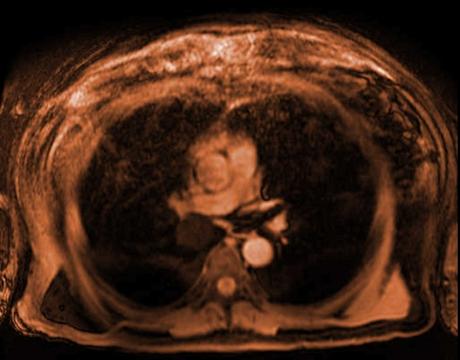
Clinical information: 3 days central abdominal pain and vomiting. Now, sudden hypotension and tachycardia with new pyrexia.
Interesting case Chest 13
.png)
.png)
Topics: Chest
Salient findings:
-
Hiatus hernia with oral contrast within the oesophagus, stomach and small bowel.
-
A nasogastric tube is seen traversing the lateral distal oesophageal wall and the tip lying in the left lower lobe.
-
Hyperdense collection of contrast lying in the medial aspect of the left lower lobe with multiple locules of gas measuring approximately 9.4 x 2.7 cm axially with atelectasis and hyperdense pleural effusion.
-
Features are consistent with perforation of the lower oesophagus with a nasogastric tube with a resultant collection and infective consolidation in the left lower lobe.
-
In addition, there are multiple dilated loops of small bowel throughout the abdomen and pelvis, mostly containing intraluminal contrast except for the distal most loops. There is a transition point in the medial aspect of the right iliac fossa with dilated loops extending back to the duodenum. Appearance are keeping with mechanical small bowel obstruction, possibly adhesional.
-
Quiescent pancolonic diverticular disease, more prominent in the ascending colon and caecum.
Principle Diagnosis: Perforation of the distal oesophagus/GOJ with a nasogastric tube resulting in consolidation and LRTI left lower lobe.
Other important findings: Small bowel obstruction with transition point in the right iliac fossa.
Learning points:
Causes of oesophageal perforation:
-
Traumatic insertion of nasogastric tube.
-
Long term siting of an NGT resulting in ulceration distally
-
Endoscopic procedures and stenting
-
Boerhaave’s syndrome (post vomiting spontaneous rupture)
-
Ingestion of corrosive foreign bodies resulting in oesophagitis
-
Oesophageal malignancy
Pros and cons of intraluminal small bowel contrast:
PRO: Due to better delineation of the bowel wall, lumen and adjacent structures, it can be easier to assess for strictures or areas of inflammation/wall thickening.
CON: Can reduce the conspicuity and preclude assessment of ischaemia because it can hide enhancement patterns of the bowel wall.
CON: It is often felt to be contraindicated in high grade small bowel obstruction because it can increase the likelihood of aspiration/ vomiting.
View our recent lectures
Related Post
-
24 April 2026
Interesting case Chest 14 Go to case -
14 August 2023
Interesting case Chest 12 Go to case -
23 May 2023
Interesting case Chest 11 Go to case
Subscribe to our content
Vivamus sagittis lacus vel augue laoreet rutrum faucibus. Paullum deliquit, ponderibus modulisque suis ratio utitur. Cum ceteris in veneratione tui montes, nascetur mus.
Latest Content
Clinical information: 36 year old male. Shortness of breath and chest pain.
Fall in shower with headache and nausea - what's the diagnosis?
Clinical information: 3 days central abdominal pain and vomiting. Now, sudden